Local 3652 Board Member Blasts NYCE PPO For Charging $877.33 for 911 Emergency Call

On January 7th Board Member Brian Cohen, Public Relation Officer called 911 for a medical emergency. This was 7 days after NYCE PPO began.
WE SHOULD NOT HAVE TO CHOOSE BETWEEN SUMMONING AN UBER OR CALLING 911 FOR AN AMBULANCE IN AN EMERGENCY.
While the MTA and not the union manage the health insurance plan this health benefit was negotiated by DC37 on behalf of its members.
We would like to crowdsource additional actions he should take in addition to contacting MTA OIG.
The below letter mentions EMS when EMT should have been used...
March 14, 2026
NYCE Post Service Appeals
PO Box 211381
Eagan, MN 55121
RE: NYCE PPO Second Level Appeal – Ground Ambulance Balance BillingMember Name: Brian Cohen, Claim Number: 2[redacted]3, Case Number: 5[redacted]9, Date of Service: January 7, 2026 Amount in Dispute: $877.83 (Provider: FDNY)
To the Plan Administrator:
I am submitting this formal second-level appeal regarding the adverse benefit determination conveyed to me on March 13, 2026. As an MTA employee and Board Member of the Metropolitan Transportation Authority (MTA) Technical Professional Employees Local 3652 (DC37), I am appealing the decision to hold me responsible for an $877.83 balance for emergency 911 transport provided by the FDNY.
1. Clinical Evidence of Emergency (Sepsis Diagnosis)
The emergency nature of this transport is indisputable. On the date of service, I began shaking uncontrollably. Fearing a life-threatening condition, my significant other contacted 911 and explicitly informed EMS upon their arrival that she was concerned I had SEPSIS. I was transported to Coney Island Hospital (a.k.a South Brooklyn Health) and immediately admitted; the attached discharge papers confirm that I did, in fact, have sepsis. Under the "prudent layperson" standard and the NYCE PPO’s "Immediate Care" definitions, this transport was a medically necessary emergency response to a critical condition.
2. The Fallacy of "Choice" and Systemic Absurdity
The previous denial states that because the FDNY is "out-of-network," the member is responsible for 100% of the balance. This is a procedural absurdity. In a 911 emergency, the caller has zero choice of provider; the dispatch system is a public safety mandate.
There is a profound and bitter irony here: It appears thatFDNY's own EMS members (Local 2507), who are also part of this plan, would then be balance-billed by the very emergency system they staff. If an FDNY EMS employee were to call 911 as a civilian during a personal medical emergency, they would then be charged nearly $900 because their own insurance labels their own employer "out-of-network." It is a logical loop of the highest order that a city employee would be charged by their own department because their insurance fails to contract with the city's primary emergency infrastructure. It is impossible for a member in septic shock to "shop" for an in-network ambulance, and penalizing them for a 911 dispatch is materially misleading.
3. Breach of Explicit Plan Language (“No Charge”)
The high-level overview of plan benefits provided to city employees (NYCE PPO Plan) explicitly states the following under "Immediate care":
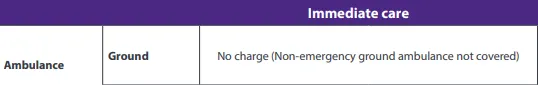
Source: https://www.nyceppo.com/print/UMC0370.pdf
The plan promises: Ambulance | Ground | No charge. By advertising "No charge" for a service where the member has zero choice in provider, and then penalizing that member for the specific unit the city dispatched, the plan is failing to honor its primary benefit summary.
4. Evidence of Failed Internal Resolution
As shown in the transcript at the bottom of this letter, from my chat with your representative, the plan acknowledged the service was processed at the "in-network level," yet still attempted to pass an $877.83 bill to the member. This internal contradiction suggests a systemic error in how emergency municipal services are being handled.
5. Notice of Formal Escalation
If this appeal is not granted and the balance is not waived, I will escalate this matter to:
The MTA Office of Inspector General (OIG) regarding the mismanagement of public employee benefits and/or The New York State Department of Financial Services (DFS).
I request that you re-process this claim, honor the "No charge" benefit as written, and hold me, the member harmless.
NYCE PPO Chat 3/13/2026:
You filed an appeal against our processing of your post-service claim; your appeal was received on March 6, 2026. This claim was for ambulance services, which were processed in-network level of benefits under the NYC Employees PPO plan.
Your adverse benefit determination has been upheld. In making this determination we reviewed the following information: your letter of appeal, the plan language/exclusion/definition/provision, our internal protocol, etc.
Colby – 2:47 PM
After review, it has been determined that the original processing of this claim is correct. Your plan benefits for ground ambulance services are paid at the in-network level; however, when the provider is out-of-network, the member is responsible for 100% of the difference between the amount billed and the plan’s allowed amount. For this claim, the provider billed a total of $1,413.00, and the plan allowed $535.17, which was paid in full according to your benefits. The remaining $877.83 represents the difference between the billed charges and the plan allowance and is the member’s responsibility under your plan provisions. Therefore, the claim was processed according to the benefit plan, no additional payment is due.
Colby – 2:47 PM
how can an ambulance sent from 911 be out of network?
i live in nyc.
You – 2:48 PM
Right to second level Appeal: We realize you may still have concerns about this decision. You may further request a voluntary second appeal by submitting a written request within 60 days to the following address: NYCE Post Service Appeals PO Box 211381 Eagan MN 55121 When requesting a review, you should state the reasons you believe the denial was improper and submit any additional information, material or comments which you consider appropriate. The Plan Administrator will review your appeal and send you a written notice of the Plan Administrator’s decision. The determination notice will include the specific reasons for the decision as well as specific references to the pertinent Plan provisions on which the decision is based.
Colby – 2:48 PM
Sincerely,
Brian Cohen
[redacted]
Brooklyn, NY [redacted]
Attachments:
- Hospital Discharge Papers (Confirming Sepsis Diagnosis).
- FDNY Ambulance Bill ($877.83).
- NYCE PPO Plan High-Level Overview.
CC w/o att (via email): Oren Barzilay (Pres. Local 2507), Executive Board (Local 3652), MTA Business Service Center, DC37 MELS Legal.
On January 7th Board Member Brian Cohen, Public Relation Officer called 911 for a medical emergency. This was 7 days after NYCE PPO began.
Since then, he filed an appeal on 3/6/26 for medical bill online and this appeal was rejected.
A second appeal (the above letter) was sent on 3/14/26 was sent via postal that was confirmed delivered to Zip Code 55121.
NYCE PPO denied ever receiving the second ) appeal letter in the mail. Moreover, he was told on 3/30/26 that a manager would call him back regarding his appeal. A manager has never called him back.
Brian has been in touch with NYCE PPO regarding this matter via
NYCE PPO Chat
NYCE PPO internal "email"
NYCE PPO Phone
And NYFD billing to provide a grace period.
